- Details
- Description
-
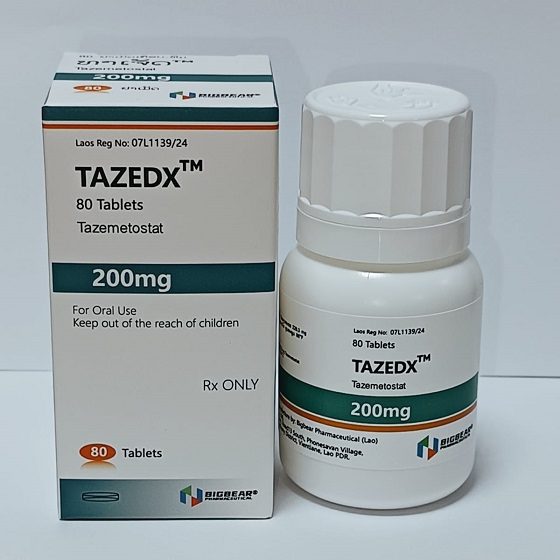
Packaging Size80t/Box
-
Strength200mg
-
CompositonTazemetostat
-
TreatmentEpithelial Sarcoma and (R/R) follicular lymphoma (FL)
-
FormTablet
-
BrandTAZEDX
-
Quantity Unit200mg*80t/Box
-
ManufacturerBIGBEAR Pharma,Laos PDR
About Tazemetostat
Tazemetostat is a selective inhibitor of EZH2, administered orally.It is approved treatment for Follicular lymphoma and epithelioid sarcoma.
Epithelial Sarcoma
Indicated for metastatic or locally advanced epithelioid sarcoma not eligible for complete resection
800 mg PO BID
Continue until disease progression or unacceptable toxicity
Follicular Lymphoma
Indicated for relapsed or refractory (R/R) follicular lymphoma (FL) in patients whose tumors are positive for EZH2 mutation and who have received at least 2 prior systemic therapies
Also, indicated for R/R FL in adults who have no satisfactory alternative treatment options
800 mg PO BID
Continue until disease progression or unacceptable toxicity
Dose reduction schedule
- First reduction: 600 mg PO BID
- Second reduction: 400 mg PO BID
- Permanently discontinue if unable to tolerate 400 mg BID